Besplatan pregled kod lekara specijaliste dermatologije ili estetske hirurgije trebalo bi zakazati ukoliko primetite bilo kakve promene na mladežu. Odnosno, ako menja boju, oblik ili veličinu.
Isto važi i ako se mladeži nalaze na mestu stalne iritacije, povređeni su ili svrbe.

Na osnovu pregleda, naš doktor procenjuje da li je potrebno:
- uklanjanje mladeža radiotalasnom tehnikom ili
- klasičnom hirurškom metodom
uz OBAVEZNU patohistološku analizu.
Naravno, moguće je zakazati skidanje mladeža i iz estetskih razloga.
Besplatne konsultacije za uklanjanje mladeža u Poliklinici Diva
BESPLATNU konsultaciju za uklanjanje mladeža u Beogradu sa lekarima poliklinike Diva dr Bogdanović možete zakazati u jednoj od naših poliklinika ili specijalističkih dermatoloških ordinacija:
- jednostavan,
- bezbolan,
- brzo izvodljiv,
- neinvanzivan i
- veoma koristan pregled mladeža,
koji lekarima specijalistima pomaže pri razlikovanju pigmentne promene na koži od melanoma.
Ova dijagnostička metoda predstavlja preoperativni pregled koji daje trodimenzionalnu sliku i pruža uvid u:
- strukturu promene,
- veličinu,
- oblik,
- oblik i raspored krvnih sudova,
- obrazac i raspored pigmenta,
- prisustvo ili odsustvo regresionih struktura ili infiltracije.
Dijagnostika pigmentnih promena i oboljenja kože
- promene na krvnim sudovima, kao i
- promene u keratinizaciji i strukturi kože
sa dijagnostičkom tačnošću od 97 do 98%.
Pravovremena i precizna dijagnoza je presudna u prevenciji tumora.
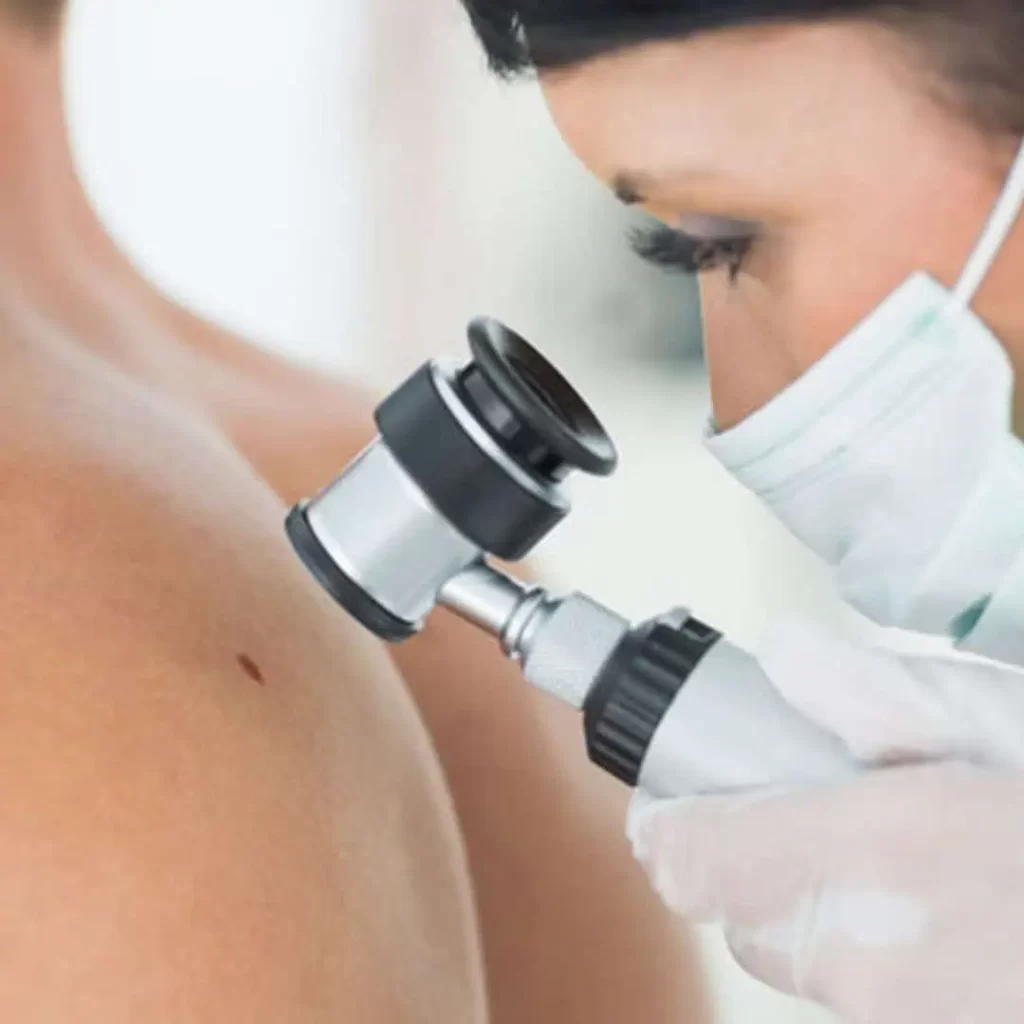
Dermoskop stvara trodimenzionalnu sliku visoke rezolucije.
Dermoskopija je neophodna za praćenje bilo koje pigmentne lezije. Sa redovnim kontrolama, posebno kod osoba s velikim brojem mladeža, najmanja promena koja nastane u mladežu može se detektovati i blagovremeno odstraniti.
Pravovremena i precizna dijagnoza je presudna u prevenciji tumora.
Zašto je važan redovan dermoskopski pregled mladeža?
Procenjuje se da je pouzdanost kliničkog pregleda mladeža (lekarski pregled „golim okom“) oko 65%. Dermoskopski pregled mladeža tačnost dijagnostike podiže i do 98% i zato igra važnu ulogu u ranom otkrivanju melanoma i drugih tumora kože.
Pouzdano razlikovanje benignih od zloćudnih promena
Kliničkim pregledom je retko dostupan uvid u oblik i strukturu krvnih sudova. To je često presudno za razlikovanje dobroćudnih od zloćudnih promena, kao i za odluku da li ona spada u grupu benignih promena, kao što su mladeži i fibromi, virusne bradavice, ili u grupu malignih promena, melanoma, bazocelularnih ili planocelularnih karcinoma, za koje je potrebno blagovremeno i radikalno lečenje.
Kakve je promene moguće dijagnostikovati pomoću dermoskopskog pregleda?
Pored pouzdanog razlikovanja benignih od zloćudnih promena, dermoskopija omogućava ranu detekciju melanoma i promena na mladežima.
Melanom – karcinom kože koji ima veliku stopu smrtnosti, ako se dijagnostikuje u kasnim stadijumima. Dijagnostika u ranoj fazi presudna je za pacijente, što nije bilo moguće pre upotrebe dermoskopskih aparata. Primera radi, u zemljama Zapadne Evrope danas se oko 80% melanoma, pomoću dermoskopskog pregleda, otkriva u ranoj fazi, što značajno povećava šanse za izlečenjem. Nakon uspostavljene sumnje na melanom, po obavljenoj dermoskopiji, vrši se uklanjanje promene na koži, a krajnja dijagnoza se postavlja posle histopatološke analize.
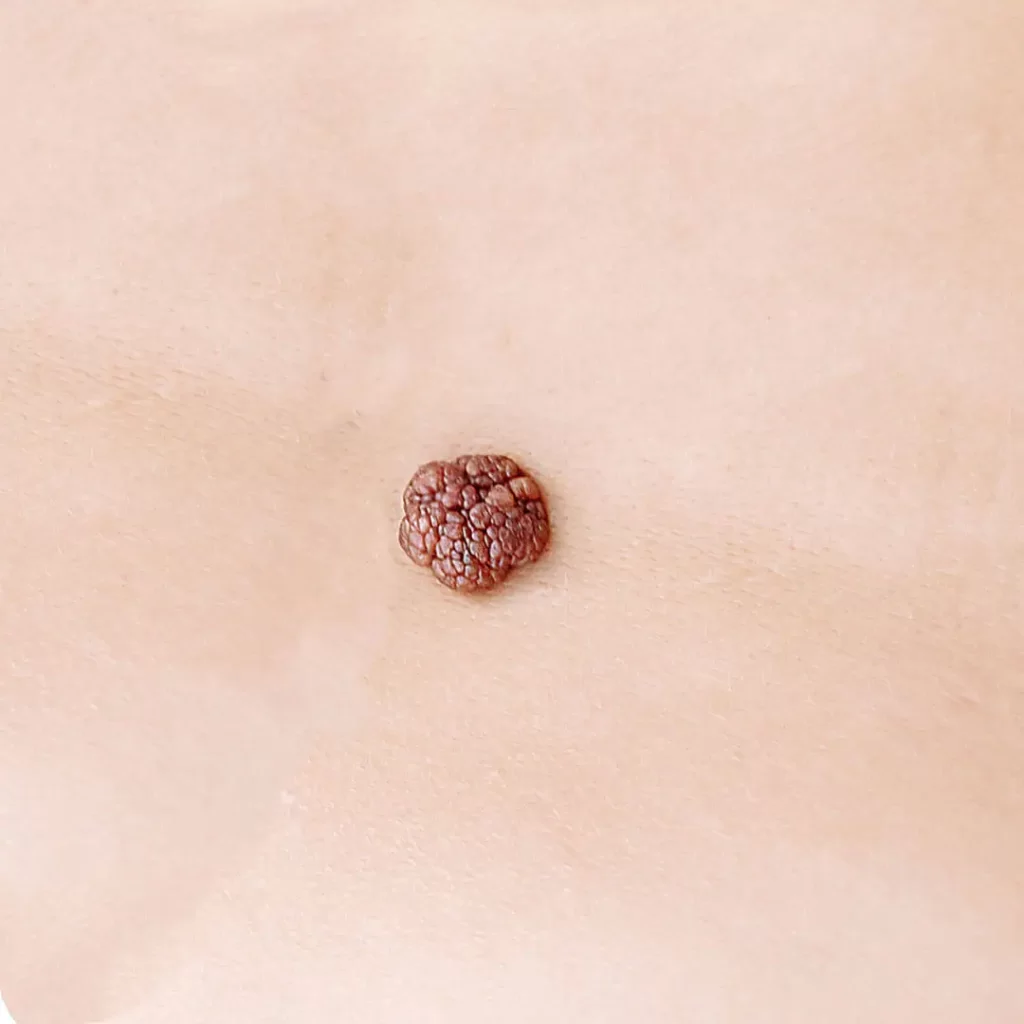
Mladež – samopregled mladeža preporučuje se na svaka 3 meseca, a dermoskopski pregled mladeža po preporuci lekara, zbog sve učestalije pojave tumora kože.
Poseban oprez za rizične grupe
Dermoskopska dijagnostika je izuzetno značajna za sve pacijente koji primete bilo kakve promene na mladežima, a posebno za visokorizične grupe pacijenata kao što su:
- pacijenti koji imaju više od 50 mladeža,
- pacijenti koji imaju displastične ili atipične mladeže,
- pacijenti stariji od 50 godina, koji imaju teška oštećenja kože prourokovana uticajem Sunca,
- pacijenti koji se često i mnogo izlažu suncu, koji se bave rizičnim profesijama, svi koji rade na otvorenom – zemljoradnici, moreplovci i drugi,
- pacijenti s porodičnim opterećenjem u smislu karcinoma ili melanoma kože,
jer ova metoda omogućava pregled čitave površine kože i praćenje na 3, 6 ili 12 meseci, prema potrebi i dinamici koju određuje lekar specijalista.
Osobe koje pripadaju nekoj od ovih visokorizičnih grupa trebalo bi da dermoskopski pregled mladeža obavljaju redovno.
Faktori rizika za nastanak tumora na koži:
- porodična predispozicija,
- prekomerno izlaganje Suncu i UV zracima u solarijumu,
- osobe sa svetloplavom ili crvenosmeđom kosom,
- veliki broj mladeža na koži,
- svetao ten i prisustvo pegica.
Koje je mladeže neophodno pregledati dermoskopskim aparatom?
Ukoliko se primećuje bilo koja od promena na mladežima, potrebna je dermoskopija. Ukoliko mladež:
- naglo raste,
- menja oblik (javlja se asimetrija),
- menja boju,
- menja ivice (one postaju iskrzane i nepravilne),
- dobija više različitih boja,
- izdiže se iznad nivoa kože tokom vremena…
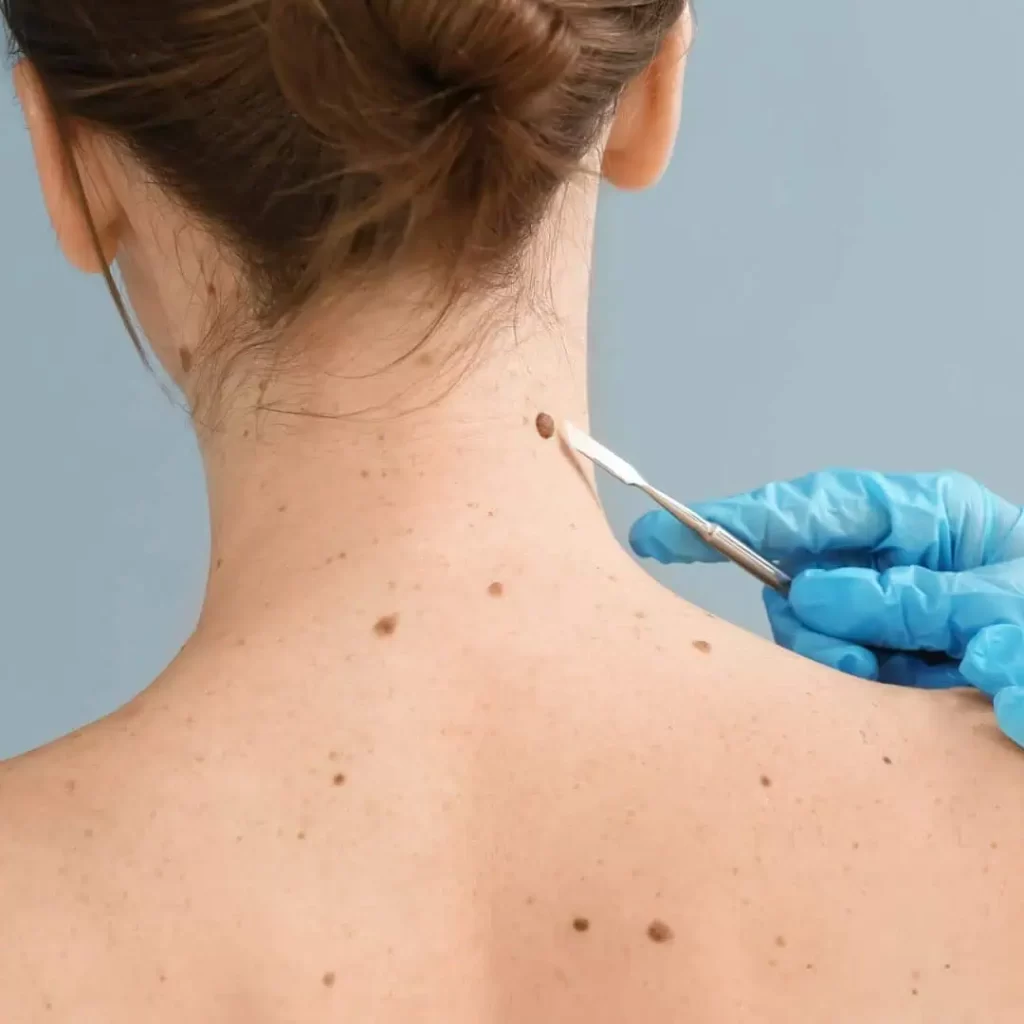
Koje je još mladeže potrebno dermoskopski pratiti?
Mladeže koji su atipičnog izgleda, čak i kada ne postoji sumnja na melanom. Oni se takođe prate na 3, 6 ili 12 meseci, nakon čega se upoređuju dermoskopske slike i donosi odluka o tome da li će biti uklonjeni, a potom urađena histopatološka analiza.
Dersmoskopski pregled se preporučuje i za praćenje urođenih kongenitalnih mladeža, naročito ako im je prečnik veći od 10 centimetara.
Dermoskopija mladeža pre intervencije – savet lekara
S obzirom na to da se beleži sve veći broj tumora, preporuka lekara je da se dermoskopski pregled mladeža obavlja barem jednom godišnje. Bradavice, mladeži i drugi izraštaji na koži mogu predstavljati potencijalna žarišta malignih tumora pa je izuzetno važna preoperativna dijagnostika aparatom za dermoskopiju, jer je presudna za isključivanje maligniteta. Tako će lekar na vreme moći da donese odluku da li je mladež potrebno ukloniti i koja bi tehnika za uklanjanje mladeža bila adekvatna.
Kojim metodama se mogu ukloniti mladeži i druge promene na koži?
U zavisnosti od vrste i veličine promene na koži i mladeža, mogu se uklanjati klasičnom hirurškom ekscizijom ili radiotalasnom hirurškom metodom, uz obaveznu histopatološku verifikaciju.
Za cene uklanjanja ostalih promena na koži pogledajte naš CENOVNIK.
Da li su radio-talasi adekvatna metoda za uklanjanje mladeža proceniće lekar specijalista na besplatnim konsultacijama.
Rezultati procedure mogu se razlikovati od pacijenta do pacijenta, a na to utiču faktori poput tipa kože, odnosno da li je sklona stvaranju ožiljačnog tkiva.
Ceo disklejmer možete pročitati OVDE.
Zakazivanje za besplatno pregledanje mladeža ili procedure za skidanje mladeža u Beogradu
U poliklinici Diva dr Bogdanović Beograd, kod naših lekara specijalista dermatologije i estetske hirurgije, možete zakazati BESPLATNU konsultaciju za pregled i uklanjanje mladeža u jednoj od naših poliklinika ili specijalističkih dermatoloških ordinacija:
na jedan od brojeva telefona 063 338 334 ili 011 3242 841 ili na mail info@divaclinic.com
Pregled ili proceduru možete zakazati
· svakog radnog dana od 9h do 20h
· i subotom od 9h do 15h.
Cena za specijalistički dermatološki pregled kože i dermoskopski pregled mladeža i drugih promena na koži
Ukoliko je potreban specijalistički dermatološki pregled kože zbog dermatoloških promena na koži tada je cena 6.000 RSD.
Ukoliko želite da zakažete samo dermoskopski pregled mladeža cena je 6.000 RSD.
Vaša „Poliklinika Diva“
Autor teksta: dr spec. Svetlana Bogdanović
Koautor: dr spec. Slavica Peković

